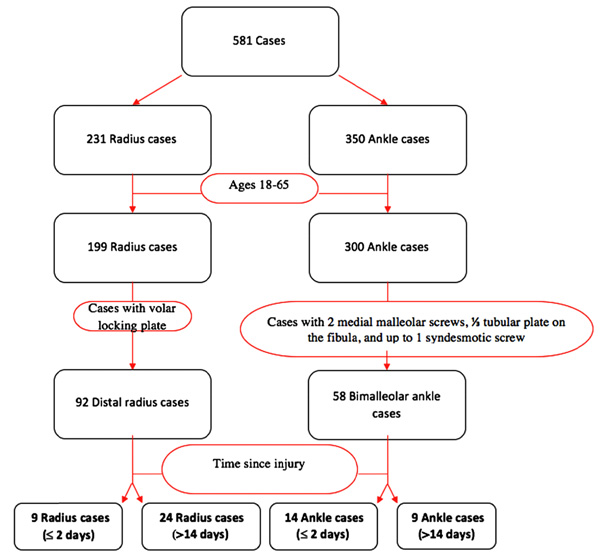
The benefit-risk balance of the various treatment options will be assessed with the main goal being that patients recover their autonomy. The treatment of bimalleolar ankle fractures in older adults requires rigorous analysis at all points, which starts by evaluating the cutaneous status and viability of the soft tissues upon admission. The functional prognosis is brought into play, along with the patient's life due to loss of autonomy and general complications occurring in patients who are bed-ridden. They can lead to complete loss of autonomy if the treatment is delayed and/or not adapted to the local conditions or the patient. Ankle injuries are particularly frequent in general traumatology but even more in geriatric traumatology. Trauma in the geriatric population involves specific risks thus, the treatment must be adapted not only to the fracture, but to the local conditions and the patient. Falls increase with age and because of certain medical conditions. Musculoskeletal injuries are common in these patients, who can maintain their physical capacities and autonomy for a long time, but whose bone solidness is frequently reduced by osteoporosis. (Simanski CJ, JOT 2006 20:108).Geriatrics continues to evolve as a specialty by adapting itself to increasingly older patients. 100% good results Olerud score (90 +/- 13 points). Average time to full weightbearing = 7weeks, return to work = 8weeks after surgery with early weight bearing protocol.Smoking history, presence of a medial malleolar fracture, lower levels of education are significant independent predictors of lower physical function up to 3 months postoperation. Physical function and role physical scores remain significantly lower than US norms at 24 months after operative fixation.6 Months: Return to sport / full activities.Running, stair-climbing, and participation in sports are allowed only after a full range of motion of the ankle has been achieved Rx=compression stocking (sigvaris, Jobst) 20-30mmHg Swelling is common after ankle sprain or fx. Driving: may drive after 9 weeks for right leg. 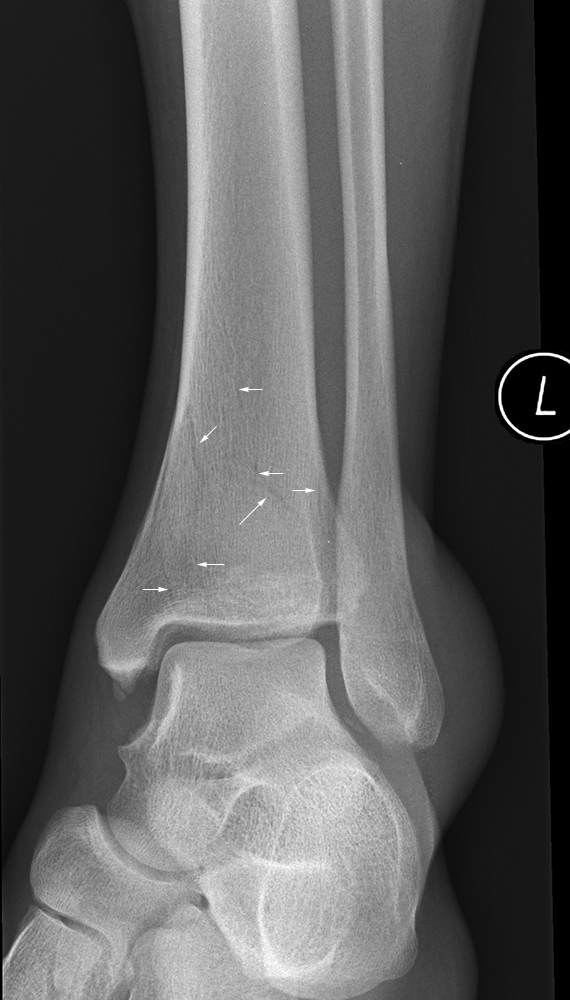
Encourage daily active and passive range-of-motion exercises of the ankle and subtalar joints without the brace. 7-10 Days: Wound check, functional Air-Stirrup ankle brace (Aircast).Post-op: bulky jones dressing, NWB, elevation.We discussed the risks of surgery including, but not limited to: incomplete relief of pain, incomplete return of function, nonunion, malnunion, painful hardware, hardware failure, compartment syndrome, CRPS, DVT/PE and the risks of anesthesia including heart attack, stroke and death.Peroneal tendon pathology: associated with low plate placement with a prominent screw head in the distal hole.Lateral malleolar fixation provided with posterior antiglide plate +/- lag screws.document osteochondral injuries which should be saught during ORIF.Prep and drape in standard sterile fashion.Well-padded tourniquet placed high on the thigh.Supine position with bump under ipsilateral hip.Pre-operative antibiotics, +/- regional block.FHL is medial and protects posterior tibial artery/nerve. Find interval between FHL and peroneal tendons. Incision between Achilles and peroneal tendons. Posterior approach only needed for large posterior malleolar fragments-prone position.Posterior malleolar fragments >25% of the plafond may be fixed via percutaneous clamp reduction through the medical mallellar fracture or direct reduction through a posterolateral or posteromedial approach.Delayed surgery done when blisters have resolved, skin wrinkles normally (average 14 days) has equivalent outcomes (Karges/Watson, JOT 1995 9:377). Ideally surgery is done before any true swelling or fracture blisters have developed. Timing of surgery is dictated by the status of the soft tissues.ORIF Ankle Fracture Pre-op Planning / Special Considerations Soft tissue compromise - severe swelling. 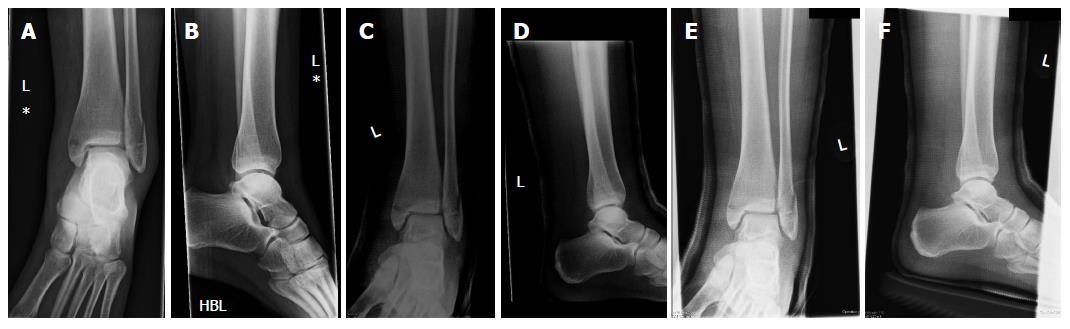
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
